Current Situation
As of April 15, 2026, a total of 37 cases of measles have been identified in Washington state this year. WA DOH is aware of at least 9 separate introductions of measles into the state since January 1, 2026, all associated with domestic or international travel. Many of these cases have led to additional local in-state transmission of measles across Washington.
Since January, measles cases identified in Washington have led to more than 50 public exposure locations where individuals may have been exposed to a person who was contagious. Additionally, at least 3 measles cases this year have not had any known links to other cases or outbreaks and report no out-of-state travel, indicating the possibility of undetected community spread of measles in Washington.
The WA DOH Measles Cases in Washington State webpage has the latest information about measles cases and outbreaks in Washington. This page also includes links to a map of active Measles Public Exposure Locations in Washington State, which shows any known public exposure locations for measles from the past 21 days
Requested Actions
IDENTIFY
- Be familiar with the three classic signs and symptoms of measles:
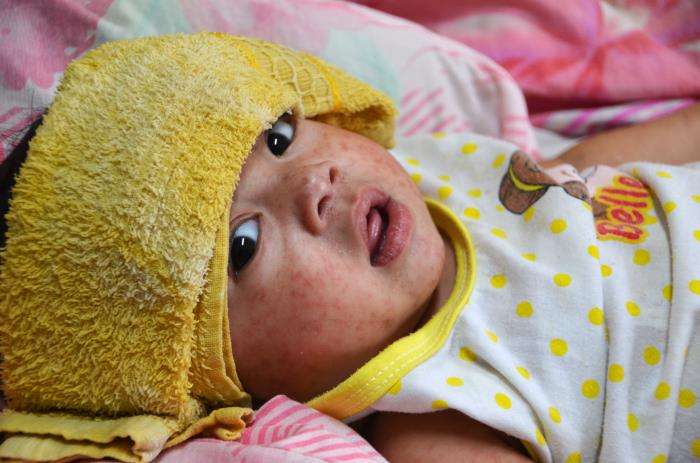
- Rash (maculopapular, confluent, starts on face and spreads down), AND Fever (101.3°F or higher, overlapping the rash onset), AND
- cough
- coryza (runny nose)
- conjunctivitis (red eyes)
- When evaluating a patient with febrile illness and rash, assess patients for measles risk factors:
- Being unvaccinated (zero doses of a measles-containing vaccine) or having unknown vaccination status
- Exposure to a case of measles within the last 21 days
- Recent travel within the past 21 days (including international AND domestic travel)
- Exposure to a known measles public exposure location in Washington in the last 21 days
- Use the WA DOH Suspect Measles Provider Evaluation Worksheet (PDF) to gather patient information and guide decision-making for measles testing.
ISOLATE
- Ensure that your facility has appropriate protocols in place to rapidly identify and isolate suspected measles cases.
- Ensure any patient with suspected measles is masked at all times.
- Patients with suspected measles should not wait in common areas, such as waiting rooms.
- Consider posting signage or instructions outside of your facility directing patients with rash and fever to call ahead for further instructions.
- As soon as measles is suspected, IMMEDIATELY:
- Isolate the patient in an airborne infection isolation room (AIIR)
- If AIIR is not available, use a private room with a closed door
- Follow Standard and Airborne Precautions when evaluating patients with suspected measles.
- Ensure health care providers wear fit-tested respirators (N95 or better) when in the patient’s airspace.
- Confirm that all health care workers that assess or care for patients with suspected or confirmed measles have documented measles immunity.
- After a patient with suspected measles is discharged, the room or area where the patient was assessed should remain vacant for at least 2 hours.
- Follow WA DOH guidance for Preventing Measles (Rubeola) in Healthcare Settings (PDF).
NOTIFY
Measles is an IMMEDIATELY notifiable condition in Washington.
- Report suspected cases of measles IMMEDATELY to Yakima Health District using the reporting line at 800-535-5016 ext. 541.
- Reports should be made by phone, at any time of day or night, including weekends and holidays.
TEST
- WA DOH offers measles testing at the Washinton State Public Health Laboratories (PHL).
- Yakima Health District can review details of the suspected case of measles and facilitate testing if appropriate.
- Refer to the Measles Specimen Testing Protocol for information about testing at PHL.
PCR (polymerase-chain reaction) testing is the preferred method to diagnose acute measles.
- Collect PCR specimens as close as possible AFTER onset of the rash, ideally within 10 days.
- Follow PHL guidance for Measles RT-PCR Specimen Collection and Submission:
o Collect nasopharyngeal (NP) or oropharyngeal (OP) swabs:
- Place swabs in Viral Transport Media (VTM) or Universal Transport Media (UTM).
- Other types of transport media used will result in rejection for testing.
- If possible, collect a urine specimen as well as an NP or OP swab.
- WA DOH advises against collecting specimens for measles testing BEFORE patients develop a rash.
- PCR specimens for measles that are collected before rash onset can NOT rule out measles; repeat testing would be required.
- Symptomatic patients without a rash who have a known measles exposure should be advised to isolate and monitor symptoms; collect measles PCR specimens if rash develops.
- Contact Yakima Health District if you have concerns for an unusual measles presentation such as modified measles or if the patient is severely immunocompromised for guidance.
- Measles testing may also be available through commercial or clinical laboratories.
- Regardless of where measles testing is completed, healthcare providers are still required to IMMEDIATELY notify Yakima Health District as soon as measles is suspected.
MANAGE
Patients with measles are contagious from approximately 4 days before through 4 days after rash onset.
- Instruct patients with suspected measles to isolate at home, even while test results are pending.
- If a suspected case of measles is confirmed in your facility:
- Coordinate with Yakima Health District and facility infection prevention program to identify any patients, staff, visitors, or others who shared airspace with the confirmed case.
- Follow WA DOH guidance for Preventing Measles (Rubeola) in Healthcare Settings (PDF).
- Post-exposure prophylaxis (PEP) for measles may be available if close contacts are identified rapidly.
- Follow WA DOH guidelines for Measles Post-Exposure Prophylaxis (PDF).
VACCINATE
MMR or MMRV remains the most important tool for preventing measles infections.
- Check WAIIS (WA State Immunization Information System) and medical records for measles vaccination or immunity status.
- Ensure all patients without evidence of immunity are up to date on measles vaccination (PDF).
- Refer to the WA DOH Interim Pediatric Measles Outbreak Vaccination Recommendations (PDF) to guide decision-making for children who live in or travel to locations with measles outbreaks.
- Ask patients about upcoming travel plans.
- If needed, offer measles vaccination at least two weeks before travel to patients with upcoming international or domestic travel.
Background
Measles is a highly contagious disease caused by the measles virus. The virus is transmitted by direct contact with infectious droplets or by airborne spread when an infected person breathes, coughs, or sneezes. Measles virus can remain infectious in the air and on surfaces for up to 2 hours after an infected person leaves an area. Measles can cause severe health complications, including pneumonia, immune system dysregulation, encephalitis, and death.
MMR vaccination remains the most effective way to protect against measles and its complications. Two doses of MMR vaccine are about 97% effective in preventing measles infections.
The United States is experiencing a rapid increase in cases of measles. As of April 10, 2026, the CDC has reported more than 1,700 cases of measles, with 9% resulting in hospitalization. In 2026, 33 states have reported cases of measles, including Washington state. For the latest information about cases of measles and outbreaks across the U.S., please visit the CDC Measles Cases and Outbreaks webpage.
Resources
- Measles and MMR Vaccine FAQ, for general information about measles, DOH
- Notifiable Conditions: Measles, for information on reporting to public health WA DOH Measles Cases in Washington State, for the latest updates about measles cases in WA, DOH
- Suspect Measles Provider Evaluation Worksheet (PDF), DOH
- Measles Public Exposure Locations in WA State, for a map of recent public exposures, DOH
- MMR Vaccine FAQ for Healthcare Providers and LHJs (PDF)
- Measles PEP for Non-Symptomatic Susceptible Contacts (PDF), DOH
- Interim Pediatric Measles Outbreak Vaccination Recommendations (PDF), DOH
- Measles Cases and Outbreaks, for the latest national measles data, CDC
- Measles Assessment Tool (MAT) for Infection Control in Healthcare Settings (PDF), CDC
