Mpox (formerly monkeypox) is a rare viral disease not often seen in the United States. Anyone can get mpox. Most people recover in 2–4 weeks, but the disease can be serious, especially for children and people who are immune compromised or pregnant.
Immediately report suspected mpox cases.
Complete and fax an intake form to our confidential fax (509) 381-3526 and review exposure guidelines to evaluate close contacts.
Call the reporting line at 800-535-5016 ext. 541 with any questions.
How to identify
It can be easy to miss mpox or mistake it for herpes, syphilis, folliculitis or an abscess.
Early symptoms
- Fever.
- Malaise.
- Headache.
- Weakness.
- Swollen lymph nodes.
Lesions
- Are well circumscribed, deep seated and often develop umbilication (dot on the top of the lesion).
- Can be extremely painful.
- Appear after fever.
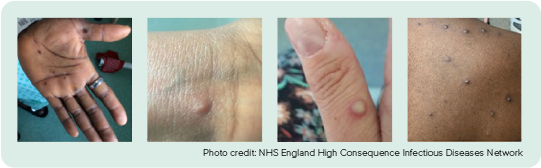
Lesions tend to appear and develop at the same time on an affected area of the body—like pustules on face or vesicles on legs. They progress through 4 stages—macular, papular, vesicular and pustular—before they scab and heal in 1–2 weeks.
Transmission
Mpox mostly spreads through close, physical contact, and is far less likely to be spread in the air.
The virus spreads through contact with:
- Mpox rash, sores or scabs.
- Objects, fabrics or surfaces a person with mpox used.
- Respiratory droplets or oral fluids from a person with mpox.
Mpox can spread as soon as symptoms start until all sores heal and a fresh layer of skin forms. This can be several weeks.
Personal protective equipment (PPE)
When you interact with a patient, wear:
- Gown.
- Eye protection (i.e., goggles or a face shield that covers the front and sides of the face).
- Gloves.
- NIOSH-approved particulate respirator equipped with N95 filters or higher.
How to test
Use a PCR test to collect a sample.
- Collect 2 swabs from each lesion on 2 separate sites. Use synthetic swabs (i.e., Dacron, polyester, nylon). Do not use cotton swabs. Vigorously swab lesions. You don’t need to de-roof the lesion before swabbing.
- Break off the end of each swab’s applicator into separate screw-capped tube or place swabs in separate sterile containers or viral transport medium (VTM). Do not use universal or other transport media.
- Store samples at 2–8° C within an hour of collection. If the testing lab won’t receive the sample within 24 hours, freeze it. Coordinate a plan with your lab manager.
Submit to a lab.
Ask your lab if they test for mpox. Follow the lab’s sample collection procedure. Labs that currently test for mpox:
- Washington State Public Health Lab (PHL). Use for uninsured patients.
- University of Washington.
- LabCorp.
- Quest.
- Aegis.
- Mayo Clinic.
Washington has no shortage of mpox tests.
How to treat
Use tecovirimat (TPOXX) antiviral medication to treat people who are at high risk of severe disease. Learn more in Centers for Disease Control and Prevention’s (CDC’s) Mpox Treatment Information for Healthcare Professionals.
Treatment and Vaccine
You should get mpox vaccine if any of the following applies to you.
- Exposed to mpox.
- Sexually assaulted.
- Male, non-binary or transgender person who has sex with men.
- Exchanged sex for money, drugs or another purpose in the last 6 months.
- Used meth in the last 6 months.
- Had an STD in the last 12 months.
- Taking PrEP to prevent HIV.
- Had multiple or anonymous sex partners in the last 6 months.
When you get vaccine, we won’t ask.
Resources
For clinicians
- Mpox page, Washington State Department of Health (DOH).
- Mpox page for healthcare professionals, CDC.
- Clinical features of mpox, CDC.
- Mpox infection prevention and control in healthcare settings, CDC.
- Mpox in animals and pets, CDC.
